The first consensual definition of Celiac Disease was published in Acta Pediátrica in 1970. Currently, it is defined as an autoimmune-based multisystemic disease caused by gluten and related prolamines in genetically susceptible individuals (HLA DQ2 or DQ8 haplotypes). It is characterized by: a series of gluten-dependent symptoms, specific to Celiac Disease, and enteropathy.
The clinical manifestations of celiac disease are varied and nonspecific, and can be digestive or extra-digestive. Sometimes, symptoms are so mild that they go undetected, talking about “asymptomatic celiac disease.” In summary, we can find different manifestations of Celiac Disease, such as:
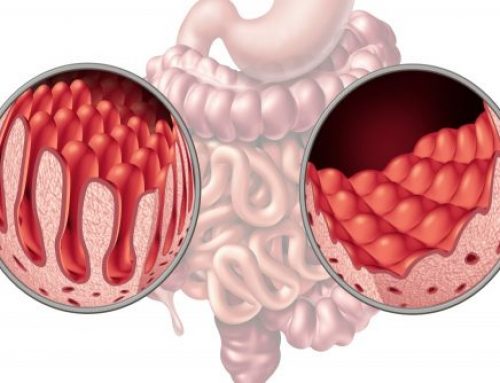
- Symptomatic or clinical: they are people with genetic predisposition and atrophy of the intestinal villi, so they will show a serology, biopsy and genetic test compatible with Celiac Disease. Among the most common symptoms we find: vomiting, diarrhea, dizziness or problems in dermis.
- Asymptomatic or subclinical: these people do not show the symptoms that are normally related to Celiac Disease, although the rest of the diagnostic tests will be positive. Thus, they have damage to the intestinal villi. Many of these people, having no symptoms, do not follow a gluten-free diet, or may suffer involuntary contamination without being aware.
- Latent: these are people who, with or without symptoms and consuming gluten, have a normal biopsy or with an increase in lymphocytes, but without reaching atrophy. Over time, they will end up with atrophy of the villi, which can subside by following a gluten-free diet.
- Potential: these are people who do not have damage to the intestine, so the biopsy is not compatible with celiac disease. However, having a genetic predisposition (HLA-DQ2 / DQ8 positivity).